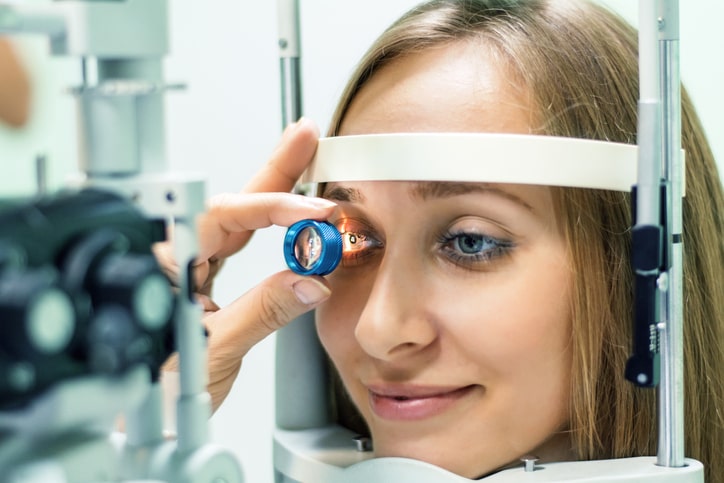
Diabetes is a complicated health issue for many people, and unfortunately, it can also lead to a number of additional health conditions that make everyday living difficult. One common health complication that can develop from diabetes is Diabetic Eye disease, a condition that affects nearly 8 million Americans.
Diabetic Retinopathy is caused by damage to the blood vessels of the retina of the eye. One of the risk factors that can lead to this problem is poorly controlled blood sugar.
Some symptoms of Diabetic Eye Disease are seeing floaters, blurred vision, dark spots, distorted vision, or altered color perception.
Diabetic eye disease can manifest in different ways. Patients may experience blurred, altered, or double vision. Diabetic macular edema, diabetic proliferal retinopathy, cataracts, and/or glaucoma can occur in diabetics.
A significant percentage of adults over the age of 45 who have been diagnosed with diabetes have had vision loss due to diabetic retinopathy. If left untreated, this disease can lead to serious eyesight issues such as poor vision or even blindness that can affect the way you see for the rest of your life. Mild cases can be treated with better diabetes management, however, more serious cases may require eye injections, laser treatment or surgery.
Dr. Stuart Sondheimer and his team are committed to helping patients with Diabetic Eye Disease. All diabetics should be examinined regularly and receive treatment with injections, lasers, or surgery when needed. We are here to help.
Interested in learning more about Diabetic Eye Disease? Read our FAQ below, or click here to contact us for a consultation today.
How Common Is Diabetic Eye Disease?
Diabetes can affect the eyes in several different ways, threatening vision. The most common condition is diabetic retinopathy. When a person has diabetic retinopathy, other eye problems such as glaucoma, cataracts, and macular edema can occur. It can also lead to a retinal detachment. All of these conditions are common when people have diabetes.
The most common diabetic eye disease is diabetic retinopathy, which is the leading cause of new cases of blindness in people ages 20 to 74 in the U.S. Nearly 1 in 3 people with diabetes will develop retinopathy at some point.
Can Diabetic Eye Conditions Be Permanently Treated?
There is no guaranteed cure for any of these diabetic eye diseases. What’s most important with each of these diseases is early diagnosis. With early diagnosis, Dr. Sondheimer often can slow or stop the progression of the disease before it impacts the patient’s vision permanently.
How Long Does It Take to Treat Diabetic Eye Disease?
Diabetic eye disease should be monitored and managed throughout the rest of your life. That’s because diabetes generally remains for life and often injures the eyes as time goes on. This is why close monitoring and meticulous treatment gives you the best chance to see for the remainder of your life. If your diabetes accelerates the development of cataracts, cataract replacement surgery only takes a few minutes and cataract lens replacement is usually a permanent vision restoration solution.
Some treatments may need to be repeated. Focal laser treatments, scatter laser treatments, and vitrectomies are all used to stem the leakage from the blood vessels abnormalities in diabetic retinopathy. Keeping your blood sugar levels under tight control will often delay the onset of diabetic retinopathy.
How Often Should a Diabetic Have His or Her Eyes Examined?
Unless advised to have more frequent examinations, every diabetic should have a complete eye examination once a year. It’s a good idea for diabetics to cover each eye for a few seconds every day and make sure that the other eye appears to be seeing well.
What Is Diabetic Macular Edema?
Diabetic Macular Edema is a thickening of the Macula (the central part of the retina that gives the clearest vision). It is caused by leakage of retinal vascular structures which are damaged by elevated blood sugar. Swelling of the macula, abnormal yellow exudates and hemorrhage in the macula. It is detected with special tests such as Ocular Coherence Tomography (OCT) and Fluorescein Angiography.
How Is Diabetic Macular Edema Treated?
Diabetic Macular Edema is treated with Intraocular Injections of anti-Vascular Endothelial Growth Factor (VEGF) medications and/or Laser treatments. The treatment stops leaking in the macula.
What Is Ischemic Diabetic Maculopathy?
Does Diabetes Cause Earlier Cataract Formation?
Yes, visually impairing cataracts are more common in diabetics than in people without cataracts. Cataracts in diabetics that cause impairment of important visual functions such as seeing to drive or read can usually be effectively treated with cataract surgery. Cataract surgery does not treat diabetic retinopathy; but sometimes cataract surgery can make it easier to treat diabetic retinopathy.
"Doctor Sondheimer is a very reliable doctor, not only does he perform finely doing his job, he really cares about his patients. I felt secured with him even though an eye surgery is considered a risk. Im so happy and blessed that I came to his office."
What Is Proliferative Diabetic Retinopathy?
In proliferative diabetic retinopathy, new abnormal blood vessels grow in the diabetic retina that can bleed, fibrose, and detach the retina. This is a condition that could dramatically affect your sight. The abnormal growth of blood vessels also increase a risk for macular edema.
How Is Proliferative Diabetic Retinopathy Treated?
Proliferative Diabetic Retinopathy is treated with laser photocoagulation, intraocular injection of anti-VEGF medication, and/or surgery to remove the vitreous gel. The goal of the treatments is to prevent any further vision loss. Controlling your blood sugar can also reduce its progression.
How Can I Prevent the Onset of a Diabetic Eye Disease?
Keeping your diabetes in control can prevent or delay the onset of diabetic eye disease. Regular examinations by Dr. Sondheimer can help detect diabetic eye and lead to earlier, more effective treatments.
When Is a Vitrectomy Required in Diabetic Eye Disease?
Surgical removal of the vitreous is necessary when blood in the vitreous does not resolve, when the retina detaches, when proliferative diabetic eye disease can’t be controlled with laser treatment, and when there is severe scarring of the retina.
What Is Recovery Like From These Surgeries?
Laser surgery for diabetic retinopathy may not restore vision that has already been lost. It often slows the progression of the disease. Your vision may be blurry for a day or so after laser surgery, but this usually clears. Your eyes may ache after treatment for several hours. . In the weeks after laser surgery, some people notice spots in their side vision when looking at objects with a white background. This should improve. If more laser treatment is needed, this can eventually cause excessive glare and difficulty seeing in sunlight.
Does Insurance Cover Diabetic Eye Treatment?
Yes. Treating diabetic eye disease is necessary to prevent potential blindness, and the diabetic evaluation and treatments used by Dr. Sondheimer are covered by insurance.
Schedule a Consultation
If you would like more information on treatment for diabetic eye problems, contact our Skokie office today! Call 847.677.2794 to schedule a consultation with top ophthalmologist Dr. Stuart Sondheimer.